research
Phenomenology of Negative Symptoms
Phenomenology of Negative Symptoms
Phenomenology of Negative Symptoms
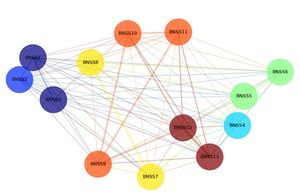
Our research on phenomenology has focused on determining: 1) whether negative symptoms are best conceptualized as a categorical, dimensional, or hybrid construct; 2) how many domains are part of the negative symptom construct. Our findings indicate that negative symptoms are a hybrid dimensional-categorical construct, such that people with schizophrenia differ in kind above a certain symptom threshold that is predictive of individual differences in the severity of several external correlates. Early work that we and others conducted on the factor structure of negative symptoms supported a two dimensional conceptualization. However, most recently, we have found that the construct is best considered in relation to 5 domains (anhedonia, avolition, asociality, blunted affect, alogia); this finding has been replicated using multiple mathematical techniques (e.g., CFA and network analysis), using multiple scales (BNSS, CAINS, SANS), across multiple cultures, both sexes, and all phases of illness (prodromal, first episode, chronic) suggesting that the 5 domain conceptualization is robust. Recently, we have been examining whether these 5 domains have distinct pathophysiological mechanisms and clinical correlates to determine whether a change is needed for DSM-5 negative symptom diagnostic criteria and whether the 5 domains reflect distinct treatment targets.
Assessment of Negative Symptoms
Phenomenology of Negative Symptoms
Phenomenology of Negative Symptoms
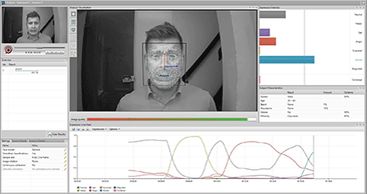
The development of next-generation negative symptom assessments has been another key focus of research in the CAN Lab. In 2005, NIMH held a consensus development conference on negative symptoms. A key conclusion of this meeting was that new rating scales were needed to increase chances of observing treatment effects. Two second generation negative symptom rating scales resulted from this initiative. Dr. Strauss was co-developer of one of these scales, the Brief Negative Symptom Scale (BNSS), and served as PI on multiple studies validating the scale. Dr Strauss has also led efforts in translating the BNSS into over a dozen languages and facilitating its primary intended use as an outcome measure in industry sponsored clinical trials. He has also begun developing and validating novel digital phenotyping measures of negative symptoms that likely reflect the third generation of negative symptom assessment (e.g., geolocation, accelerometry, ambient sound, measures of facial and vocal affect recorded from ambulatory videos). We are pioneering big data analytic approaches for evaluating digital phenotyping data.
Etiology of Negative Symptoms
Phenomenology of Negative Symptoms
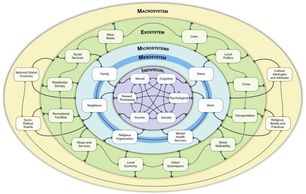
The primary focus of our research is on identifying mechanisms underlying negative symptoms. Our initial studies examined the most straightforward explanation for avolitional symptoms in schizophrenia- that individuals fail to engage in activities because they do not find them rewarding; however, this hypothesis was not supported because subjective and neurophysiological response to rewarding stimuli is intact in schizophrenia. This finding lead us to explore why apparently normal hedonic responses do not translate into goal-directed behavior in schizophrenia. We have demonstrated that abnormalities in several aspects of reward processing (e.g., reinforcement learning, effort-cost computation, value representation, uncertainty-driven exploration) that are driven by aberrant cortico-striatal interactions may prevent intact hedonic responses from influencing decision-making processes that are needed to initiate motivated behavior. We have also demonstrated that avolition is associated with dysfunctional cognition-emotion interactions (e.g., memory, attention), emotion regulation abnormalities, social cognition impairments, a reduction in the positivity offset, and anhedonic beliefs. Most recently, we are exploring a novel "bioecosystem" theory of negative symptoms that proposes interactions between person-level biological and psychological factors with environmental systems (microsystem, mesosystem, exosystem, and macrosystem) that cause or maintain negative symptoms.
Treatment of Negative Symptoms

In collaboration with colleagues in psychiatry, Dr. Strauss has conducted clinical trials examining the efficacy of pharmacological treatments for negative symptoms. Based on our studies showing a role for endogenous oxytocin in social cognition deficits and negative symptoms, we examined the efficacy of oxytocin as a treatment for asociality. In two trials, oxytocin was not more effective than placebo, and we recently extended this work by demonstrating that combining oxytocin with psychosocial treatment has no added benefit over psychosocial treatment alone. In collaboration with the pharmaceutical industry, we have examined the symptom network structure that predicts successful treatment of negative symptoms. In a phase 2B study of Roluperidone, we found that avolition was the most central symptom for the treatment of negative symptoms- when motivational deficits were successfully targeted, a casscadidng effect was seen in terms of improvement in the other 4 domains: asociality, anhedonia, blunted affect, alogia. This was replicated in the Phase 3 roluperidone trial. We have also explored the efficacy of a cognitive behavioral mHealth intervention for negative symptoms using a novel app-based therapy.
Psychosis Risk

In the past few years, we have expanded our work on the phenomenology, etiology, assessment, and treatment of negative symptoms into the psychosis prodrome. In the Georgia and Illinois Negative Symptom Study (GAINS) R01, we developed and validated a new scale for those at clinical high-risk for psychosis, the Negative Symptom Inventory- Psychosis Risk. Individuals at clinical high-risk for psychosis are best fit by a 5 factor and hierarchical model, suggesting similar underlying factor structure to schizophrenia. In our studies examining negative symptom mechanisms, we have found that reward processing deficits predict the severity of negative symptoms in youth at clinical high-risk for psychosis. However, due to the greater propensity for depression in this phase of illness, hedonic deficits play a greater role in negative symptoms in the prodrome than in schizophrenia, propagating forward and creating deficits in other aspects of reward processing that also occur in schizophrenia. We are currently conducting longitudinal studies to determine which reward processing mechanisms associated with negative symptoms predict the emergence of psychotic disorders versus other conditions (e.g., depression) in youth at clinical high-risk for psychosis in the CAPR R01. This study also seeks to develop a symptom sensitive online cognitive task screening battery that can index level of psychosis risk.
Emotion Regulation

Our research on emotion regulation aims to delineate the nature of emotion regulation abnormalities at various stages (identification, selection, implementation, monitoring dynamics) across phases of psychosis. We find a similar profile in prodromal and chronic illness phases, characterized by a low threshold for identifying the need to regulate, difficulty selecting contextually appropriate strategies, less effective implementation, and greater rates of switching and stopping regulatory attempts. Using EMA, EEG, fMRI, and eye tracking, we find evidence for moderators of these stage-specific abnormalities, such as effort allocation, prefrontal-amygdala coupling, dysfunctional patterns of attention, and emotional awareness.In an R61 grant from NIMH, we recently showed that an emotion regulation intervention delivered over an app can augment some of these underlying mechanisms, increasing attentional control and prefrontal activation. In the R33 phase of the grant, we are examining whether mechanism engagement can be replicated in a subsequent study and whether prefrontal activation enhancement predicts subsequent improvement in symptoms.
Our Methods
Electroencephalography (EEG)
Electroencephalography (EEG)

We use EEG to examine the time-course of neural activity in relation to various emotional and cognitive processes. EEG involves recording electrical activity along the scalp. EEG measures voltage fluctuations resulting from ionic current flows within neurons. In our studies, we have primarily been interested in Event Related Potentials (ERPs), which are averaged EEG responses that are time-locked to stimuli in an experiment. For example, we have examined time-locked response to pleasant, unpleasant, and neutral images to explore the time-course of affective response in people with schizophrenia compared to controls. Our EEG studies are conducted within our laboratory in the Psychology Department. We have three 64-channel Brain Vision ActiChamp Systems. We have been using EEG/ERPs since 2010.
Eye Tracking
Electroencephalography (EEG)

We use eye-tracking to measure the role of visual attention in various cognitive and emotional processes. We do this by measuring point of gaze or motion of the eyes relative to the head and a stimulus presented on the computer screen using an eye-tracker. The eye-tracker monitors the position of the pupil, pupil size, and corneal reflection as a participant views images on the screen. We have used eye-tracking to explore individual components of attention and how they interact with emotional vs. neutral stimuli in people with schizophrenia and controls. We are also interested in how pupil dilation is impacted by various manipulations of emotion and cognitive load. Our lab has two SR Research Eyelink 1000 systems that are used to measure attentional allocation and pupil dilation. This desktop mounted system allows for a remote and headfree evaluation of eye-movements at a very high sampling rate. We also interface EEG/ERPs and eye-tracking in the lab and fMRI and eye tracking at the BIRC. We have been using eye tracking since 2004.
Functional Magnetic Ressonance Imaging (fMRI)
Functional Magnetic Ressonance Imaging (fMRI)

Our fMRI studies are conducted at UGA's Biomedical Imaging Research Center (BIRC): https://birc.uga.edu/. The BIRC houses a state-of-the-art, General Electric 32-channel fixed-site Signa HDx 3.0 Tesla Magnetic Resonance Imaging (MRI) magnet. The magnet makes available multiple magnetic resonance imaging techniques including magnetic resonance imaging for structural tissue imaging (MRI), functional neuroimaging (fMRI) for studies of brain activation in real time, magnetic resonance spectroscopy (MRS) for the study of chemical changes in the brain, and magnetic resonance angiography (MRA) for the study of vascular changes throughout the system. Multinuclear spectroscopy (MNS) is available for enhanced spectroscopic studies and includes phosphorous-31. We have been using fMRI since 2019.
Psychophysiology
Digital Phenotyping
Functional Magnetic Ressonance Imaging (fMRI)

We use the wireless Bionomadix recording system from Biopac to examine facial electromyography, respiration, heart rate, and skin conductance. These psychophysiological measures allow us to explore the timecourse of psychophysiological response in relation to emotional reactivity and emotion regulation tasks, as well as the coherence between subjective, neural, and peripheral psychophysiological response when used in conjunction with our other measures. We use the wireless bionomadix system in our studies involving social interaction, as well as more traditional computerized laboratory paradigms examining emotion. We have been using peripheral psychophysiology since 2013.
Digital Phenotyping
Digital Phenotyping
Digital Phenotyping
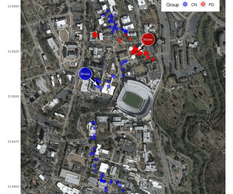
We use digital phenotyping to explore symptoms and their mechanisms as they occur in everyday life. Participants are asked to carry a smart phone and wear a digital band that collects psychophysiology for several days in the context of everyday life. Participants report their current activities, as well as their emotional experience during those activities at several points throughout the day. The internal sensors of the phone also passively collect objective data related to behavior via measurements of accelerometry, geolocation, and ambient sound. Participants also record brief videos on the cell phone that are later submitted to automated algorithms for processing facial and vocal affect. We are using these digital phenotyping methods to explore hypotheses related to negative symptoms, as well as the reliability and validity of active and passive data collection methods as third-generation negative symptom measures. We have been using digital phenotyping since 2015.
Blood Draw/Saliva
Digital Phenotyping
Digital Phenotyping
We obtain salivary and blood samples to test hypotheses related to neuroendocrine (e.g., cortisol) and immune (cytokines) function in relation to task performance. Salivary samples are obtained and stored in a -40 freezer located in our lab in the Psychology building. Blood samples are obtained and stored at the Clinical Translational Research Unit on the UGA Medical School campus. We have been gathering saliva/blood draws since 2010.
Grant Funding
National Institute of Mental Health
Brain & Behavior Research Foundation
National Institute of Mental Health

National Science Foundation
Brain & Behavior Research Foundation
National Institute of Mental Health

Brain & Behavior Research Foundation
Brain & Behavior Research Foundation

American Psychological Foundation

VA MIRECC
UGA Internal

UGA Internal
UGA Internal

ACTIVE
4. R33-MH121560 (PI GP Strauss) 04/01/2020 – 03/31/2025
NIMH $2,997,345
Cognitive training for emotion regulation in psychotic disorders.
This grant examines the efficacy of a novel app-based cognitive training program for enhancing the proximal target of emotion regulation via a direct mechanistic effect on increasing prefrontal activation, as well as a distal target of improving symptoms and functional outcome.
Role: PI
3. U01MH124639 (PI: SW Woods) 09/08/2020-06/30/2025
NIMH $1,732,983; Total funding across all sites: $52,000,000
ProNET: Psychosis Risk Outcomes Network
This multinational study evaluates biomarkers and clinical factors giving rise to the development of psychotic disorders in those at clinical high-risk for psychosis
Role: Site PI
2. R01-MH120092 (PI: GP Strauss) 04/01/2020-03/31/2025
NIMH $2,080,177
4/5 CAPER: Computerized Assessment of Psychosis Risk
This grant develops and validates a novel computerized screening battery for the early identification of psychosis among youth with prodromal syndromes.
Role: PI
1. R01-MH116039 (PI GP Strauss) 03/01/2019-11/30/2025
NIMH $2,969,883
Prodromal Inventory for Negative Symptoms (PINS): A Development and Validation Study
This grant develops and validates novel methods for assessing negative symptoms in youth at clinical high-risk for psychosis to enhance risk prediction algorithms
Role: PI
COMPLETED
21. R61-MH121560 (PI GP Strauss) 04/01/2020 – 03/31/2025
NIMH $2,997,345
Cognitive training for emotion regulation in psychotic disorders.
This grant examines the efficacy of a novel app-based cognitive training program for enhancing the proximal target of emotion regulation via a direct mechanistic effect on increasing prefrontal activation, as well as a distal target of improving symptoms and functional outcome.
Role: PI
20. R21 –MH122863 (PI: GP Strauss) 04/01/2020-03/31/2023
NIMH $440,650
Computationally modeling the failure of effort to become a secondary reinforcer in schizophrenia
This grant uses computational modeling and pupillometry to test the novel hypothesis that avolition in schizophrenia results from a failure of effort to become a secondary reinforcer
Role: PI
19. F31-MH125563 (PI: L.A. Bartolomeo) 05/24/2021-07/31/2023
NIMH $80,476
The neural basis of the positivity offset as a mechanism for avolition in schizophrenia
This NRSA pre-doctoral mentored fellowship focuses on using fMRI to identify the neural mechanisms underlying avolition as a reduction in the positivity offset.
Role: Mentor
18. (PI: Luther, L.) 09/01/2021-11/1/2022
American Psychological Foundation $19,726
Neural predictors and changes in relation to an mHealth intervention in psychosis.
This study evaluates the efficacy of a novel mobile health intervention for negative symptoms by determining whether alterations in reward circuitry as measured via fMRI act as a mechanism of action.
Role: Mentor
17. R21-MH119438 (PI GP Strauss) 09/01/2019-06/30/2023
NIMH $415,250
Mechanisms Underlying Emotion Regulation Abnormalities in Youth at Clinical High-Risk for Psychosis
This grant examines mechanisms underlying emotion regulation abnormalities at the identification, selection, and implementation stages in youth at clinical high-risk for psychosis using EMA, ambulatory psychophysiology, EEG, pupillometry, and eye-tracking.
Role: PI
16. R01MH116039-02S1 (PI: Ivan Ruiz) 12/01/2019-11/30-2021
NIMH $116,282
Prodromal Inventory for Negative Symptoms (PINS): A Development and Validation Study
This diversity supplement awards a fellowship for Strauss lab graduate student Ivan Ruiz to conduct a sub-study on cognitive effort mechanisms of avolition in youth with prodromal syndromes and obtain additional clinical and neuroscience based training.
Role: Mentor
15. NARSAD Young Investigator Grant (PI GP Strauss) 01/15/2019-01/15/2021
Brain & Behavior Research Foundation $70,000
Neurocomputational models of psychosis risk
This grant uses computational modeling approaches to examine mechanisms underlying positive and negative symptoms involved with conversion to a psychotic disorder in youth at clinical high-risk for psychosis.
Role: PI
14. R21- MH112925 (PI GP Strauss) 04/01/2017- 03/31/2020
NIMH $417,456
Modeling anhedonia in schizophrenia: A stochastic dynamical systems approach
This grant applies mathematical models to ecological momentary assessment data to test novel theories about anhedonia reflecting abnormalities in the temporal dynamics of emotion in schizophrenia.
Role: PI
13. University of Georgia (PI GP Strauss) 10/15/2017-6/30/2019
Clinical Translational Research Unit Pilot Grant $25,200
The Effects of Inflammation on Neurocomputationally Derived Reinforcement Learning Profiles in Schizophrenia
This grant examines whether cytokines predict computationally derived measures of reinforcement learning in schizophrenia to index the contributions of inflammation to negative symptoms.
Role: PI
12. University of Georgia (PI GP Strauss) 11/01/2017-06/30/2017
Owens Institute for Behavioral Research Pilot Grant $10,000
Neurocomputational Models of Reinforcement Learning in Youth at Clinical High-Risk for Psychosis
The study examines a computational neuroscience framework for understanding delusions and avolition in youth at clinical high-risk for psychosis using computational models of reinforcement learning.
Role: PI
11. NSF Graduate Research Fellowship (PI: KH Frost) 08/31/2015-08/30/2018
National Science Foundation $105,600
The Effects of Acute Social Stress on Reward Processing in Humans
This mentored grant examines sex differences in the effects of acute social stress on reward processing in humans, including implicit reinforcement learning, prediction error signaling, value representation, reward anticipation, reward consummation, effort-cost computation, and action selection.
Role: Mentor
10. R34-MH100362 (PI: RW Buchanan) 3/31/13 – 3/31/2016
NIMH $690,750
Combined Oxytocin and CBSST for Social Function in People with Schizophrenia
The study examines the efficacy of oxytocin combined with cognitive behavior therapy social skills training (CBSST) at improving social outcome in people with schizophrenia.
Role: Co-Investigator
9. Wechsler Early Career Grant for Innovative Work in Cognition 10/01/2015-2/30/2017
American Psychological Foundation (APF) $25,000
A Cognitive Neuroscience Account of Low Cognitive Effort in Schizophrenia
This grant explores a novel account of low effort in schizophrenia as resulting from failure to detect cognitive demands and adjust effort levels accordingly to maximize cognitive performance.
Role: PI
8. Interdisciplinary Collaborative Grant (PI: GP Strauss) 05/01/2015 – 12/30/2016
State University of New York $10,000
Using Network Analysis to Explore the Temporal Dynamics of Emotion in Schizophrenia.
This study uses network analysis to Ecological Momentary Assessment data in people with schizophrenia to determine whether anhedonia reflects abnormal temporal dynamics of emotional experience.
Role: PI
7. Transdisciplinary Areas of Excellence Grant (PI: GP Strauss) 05/01/2015-12/30/2016
State University of New York $20,000
Predicting Conversion to Psychosis in At-Risk Youth: The Role of Stress-Inflammation Interactions.
The study examines whether biomarkers of stress and inflammation following an acute social stressor predict symptoms of attenuated psychosis and conversion to a psychotic disorder in at-risk youth.
Role: PI
6. K23-MH092530 (PI: GP Strauss) 09/08/10 – 09/30/2015
NIMH $796,699
Motivated Attention and Avolition in Individuals with Schizophrenia
The study examines early emotion processing abnormalities in schizophrenia, and attempts to identify precise cognitive mechanisms that contribute to abnormal attention-emotion interactions in schizophrenia. Career development activities include training in Event Related Potential and Eye-Tracking technology, as well as the theoretical basis of cognitive/affective neuroscience.
Role: PI
5. Department of Veterans Affairs (PI: GP Strauss) 10/01/2011 –09/30/2013
MIRECC VISN 5 $50,000
Oxytocin and Social Cognition in Schizophrenia
The study examined the role of the oxytocin receptor gene and plasma oxytocin levels in deficits in social cognition, emotional experience, emotion perception, and emotional memory in people with schizophrenia.
Role: PI
4. Department of Veterans Affairs (PI: GP Strauss) 10/01/2012 –09/30/2013
MIRECC VISN 5 $25,000
A Study of Subjective Emotional Experience and Emotion Regulation in Schizophrenia using an Experience Sampling Approach
The study used experience sampling methodology to examine differences in prospective, retrospective, and in-the-moment reports of positive and negative emotion in people with schizophrenia and healthy controls, as well as the effectiveness of various emotion regulation strategies in the context of every-day life.
Role: PI
3. Department of Veterans Affairs (PI: GP Strauss) 10/01/2010 –09/30/2011
MIRECC VISN 5 $25,000
Cognitive Behavioral Social Skills Training to Enhance Consumer Recovery in
Schizophrenia
The study examined the efficacy of Cognitive Behavioral Social Skills Therapy enhanced with new techniques that foster optimism, hope, mastery, empowerment, and self-esteem for consumer-oriented recovery in schizophrenia.
Role: PI
2. T32-MH067533 (PI : WT Carpenter) 07/01/2010-06/30/2015
NIMH $106,515
Multidisciplinary Schizophrenia Research Training
The major goals of the project are to provide young investigators with research training in
schizophrenia research to facilitate their goals of becoming an independent investigator.
Role: Co-Investigator
1. P50-MH082999 (PI: WT Carpenter) 09/01/08- 08/31/12
NIMH $9,708,330
MPRC Centers for Intervention Development and Applied Research (CIDAR)
This application proposes to establish a Center for Intervention Development and Applied Research (CIDAR) in response to PAR-05-039. Its focus will be to advance drug discovery using innovative evaluation platforms and testing drugs with novel molecular targets to address negative symptoms and cognitive impairments in schizophrenia.
Role: Co-Investigator
Measures
Brief Negative Symptom Scale (BNSS)

The BNSS is a 13-item psychiatric rating scale designed to assess the negative symptoms of schizophrenia. The scale is rated after completing a 15-minute interview. The BNSS includes a brief but comprehensive 9 page manual, a workbook to be used when conducting the clinical interview, and a scoresheet. In multiple psychometric studies, the BNSS has demonstrated excellent inter-rater agreement, internal-consistency, test-retest reliability, convergent validity, and discriminant validity. It produces a 5 factor solution for the domains of anhedonia, avolition, asocality, restricted affect, alogia. The BNSS has been, or is currently in the process of being translated into several languages, including: Spanish, Italian, German, Cantonese, French, Korean, and Turkish. Individuals interested in obtaining BNSS materials and publications can visit our Resources page. Commercial entities wishing to use the BNSS in clinical trials can contact Prophase, which offers professional BNSS training that was developed in consultation with the test developers. Drs. Strauss and Kirkpatrick receive royalties and consultation fees from Prophase LLC in connection with commercial use of the BNSS and other professional activities. Individual researchers/research groups may use the BNSS free of charge and obtain training materials by contacting Dr. Strauss gstrauss@uga.edu or Dr. Kirkpatrick bkirkpatrick@unr.edu
Negative Symptom Inventory-Psychosis Risk (NSI-PR)

The NSI-PR is a new measure that was developed via a multi-site collaborative R01 from NIMH as part of the Georgia and Illinois Negative Symptom Study (GAINS). The study is conducted in the laboratories of Dr. Gregory Strauss at UGA, Dr. Vijay Mittal at Northwestern, and Dr. Elaine Walker at Emory University. The final measure was developed as part of an iterative data-driven process based on multiple studies. It is currently being validated as part of the GAINS R01 and will be used in the multi-site ProNet U01. It is an 11 item clinical rating scale designed to assess negative symptoms in the prodromal phase of illness specifically. The scale is rated after a 15 minute interview. Materials include a manual, interview guide, scoresheet, and frequently asked questions sheet. A powerpoint introductory training lecture and instructional training videos are also available upon request. To obtain the latest version please email Dr. Strauss gstrauss@uga.edu or Dr. Mittal: vijay.mittal@northwestern.edu.
Digital Phenotyping
Digital Phenotyping

We are developing and validating a number of novel digital phenotyping methods for assessing psychiatric symptoms. These involve active methods (e.g., daily surveys, cognitive tests, videos) completed by the participant on the phone, as well as passive methods that involve unobtrusively recording objective measures of symptoms via the internal sensors of the phone (e.g., geolocation, accelerometry, ambient sound). Contact Dr. Strauss at gstrauss@uga.edu for details.